When your cat is suffering from frequent vomiting, chronic diarrhea, weight loss, or other uncomfortable digestive issues, you want to know what’s wrong and how to fix it. But after ruling out several of the most common explanations for these symptoms (like parasites, food sensitivities, and hyperthyroidism), your veterinarian may conclude that your cat has a condition called inflammatory bowel disease (IBD). What exactly is IBD? What causes it? And what’s the best way to help your cat feel better?
What is Feline Inflammatory Bowel Disease?
Inflammatory bowel disease is a condition in which inflammatory cells penetrate the wall of the intestine, causing the gastrointestinal (GI) tract to become inflamed (irritated and swollen). This can interfere with important digestive and immune functions of the gut. Feline IBD is a common disorder, particularly in older cats and those with certain genetic predispositions.
Is IBD the Same as IBS in Cats?
Inflammatory bowel disease is sometimes confused with irritable bowel syndrome (IBS), a term reserved for gastrointestinal disorders in human patients. You may also hear the term “stress colitis,” which is used to describe acute (sudden, short-term) disturbances of the colon caused by stress.
Although IBS and “stress colitis” share some of the outward signs of IBD (symptoms like diarrhea and vomiting), intestinal biopsies of patients with IBS and “stress colitis” fail to show inflammation.
Colitis literally means “colon inflammation,” which is confirmed by the finding of excess inflammatory cells within the colon walls. In IBD, inflammatory cells infiltrate the intestinal wall, leading to inflammation of the colon (colitis), the small intestine (enteritis), and/or the stomach (gastritis).
Your veterinarian (DVM) may also use the term chronic enteropathy, which is a broader category encompassing all chronic issues related to the GI tract of pets.
What Are the Clinical Signs of IBD In Cats?
While the symptoms of IBD depend on the location and severity of the inflammation, these are the most common clinical signs in cats:
- Chronic diarrhea
- Frequent vomiting
- Blood in the stool
- Weight loss
- Decreased appetite
- Lethargy
- Mucus in the stool
- Bloating
- Straining in the litter box
Is IBD in Cats Painful?
IBD can cause pain, such as abdominal cramping from diarrhea. However, a cat with IBD is more likely to experience discomfort rather than severe pain. For example, in some cases of IBD, cats may vomit hairballs because an inflamed digestive tract can’t move material along properly.
A cat who uncharacteristically protests when picked up may have abdominal pain. Keep an eye out for this kind of behavior, and contact your veterinarian if you ever suspect your cat is in pain.
How IBD is diagnosed: What to Expect at the Vet
When you bring your cat to the veterinarian for possible IBD, you can expect a thorough evaluation to help identify the underlying cause of persistent digestive symptoms.
Your vet will begin by taking a detailed history and performing a comprehensive physical exam, paying special attention to signs such as abnormal stools, unexplained weight loss, or chronic vomiting. Several conditions can result in symptoms similar to those of IBD, including intestinal parasites, GI infections, food allergies, and metabolic diseases. Therefore, your veterinarian may recommend bloodwork to assess organ function and identify signs of systemic illness, as well as vitamin B12 (cobalamin) levels, since deficiencies are common with chronic intestinal inflammation.
Depending on your cat’s unique case, a number of tests may be recommended to determine the root cause of symptoms. Stool tests, ultrasounds, and radiographs can help rule out infections, blockages, tumors, or physical problems with internal organs. In many cases, a diet trial featuring a novel protein or a hydrolyzed diet may be conducted to identify food sensitivities or allergies. If these tests do not reveal the underlying cause of symptoms, a definitive diagnosis of feline IBD relies upon a biopsy (small tissue sampling) of the intestines. This tissue sample is evaluated to determine whether the cat may have IBD, intestinal lymphoma, or something else.
Throughout the diagnostic process, open communication with your veterinary team is vital—they can help interpret test outcomes, discuss the rationale for each step, and provide guidance on the next appropriate actions to optimize your cat’s health.
IBD Treatment: How to Restore Your Cat’s Gut Balance

The primary goal of any treatment for IBD is to reduce the inflammation of the GI tract. For this reason, steroids like prednisolone (or the related drug prednisone) and budesonide are often prescribed for their anti-inflammatory properties. Antibiotics such as metronidazole are also commonly prescribed, because they can have an anti-inflammatory effect when used long-term.
However, steroids and antibiotics typically won’t resolve the underlying cause of inflammation, and can lead to further adverse side effects. The best treatment for your cat’s IBD will depend on your cat’s individual case, and finding the optimal approach may take a bit of trial and error. Remember that diet, the gut microbiome, environmental elements, and your cat’s genes (or a combination of these factors) may be strongly influencing your cat’s IBD.
The good news is that you can do a lot to help manage your cat’s IBD by making positive changes to your cat’s diet and gut microbiome.
Dietary Changes
Diet is the most effective way to manage your cat’s gut health. What you feed your cat determines what their gut bacteria eat too.
Food Trials
A very common factor in gut inflammation is a cat’s diet. As a cat gets older, their dietary needs change, and they can also develop food sensitivities or allergies to common ingredients in cat foods, especially if they have eaten the same food for many years.
Your veterinarian may suggest a food trial using a novel protein (a protein source your cat has never eaten before) or a hypoallergenic prescription diet to see if your cat’s symptoms improve.
Some cats with chronic diarrhea benefit from added fiber in their diet, so ask your veterinarian about the best kind of fiber to use (inulin is especially good for cats) and how to introduce it gradually into your cat’s diet. Many IBD pet parents have seen symptoms improve significantly with dietary therapy or a customized feline IBD diet.
Vitamin B12 Injections
Supplementing your cat’s diet may be necessary to help relieve symptoms of IBD, especially in more severe cases. Gut inflammation may affect the absorption of vitamin B12, which is essential to digestion and cell signaling, so subcutaneous injections of B12 (also called cobalamin) may be necessary to resolve or prevent a deficiency in this vitamin. Many cats benefit from weekly injections or oral doses of vitamin B12.
Prebiotics
Prebiotics, which are particular kinds of dietary fiber molecules, promote the growth of beneficial bacteria in your cat’s digestive tract. Prebiotics have also been found to help counteract the inflammation caused by a high-fat diet.
Different bacteria eat different things, so by feeding the right prebiotics, you can encourage the kinds of gut bacteria that will improve and support your cat’s digestive health. Examples of these prebiotic fibers are inulin, mannan-oligosaccharides (MOS), and fructo-oligosaccharides (FOS). FOS has the advantage of being especially palatable to cats.
Probiotics
There are countless probiotic supplements that claim to help with IBD, although the effectiveness of specific strains of probiotic bacteria for reducing gut inflammation in humans is unclear.
Some probiotic products marketed for cats may temporarily improve diarrhea, but they can’t rebalance a disrupted microbiome. That’s because these products tend to contain large quantities of just a few kinds of bacteria, and they’re typically not bacteria that are native to the feline gut.
One probiotic we do recommend is Saccharomyces boulardii. S. boulardii is not a type of bacteria. It’s a beneficial strain of yeast that has been extensively studied for its probiotic effects. S. boulardii been shown to be especially effective at resolving diarrhea in pets with chronic intestinal disease.
Our S. boulardii + FOS Powder combines this probiotic yeast with the prebiotic FOS to improve stool consistency, reduce diarrhea, and support healthy gut function.
Treating IBD with Fecal Microbiota Transplantation
Because gut microbiome imbalance (dysbiosis) is now widely recognized as a prominent feature of IBD, new approaches to treating this disease focus on restoring balance in the gut.
The most effective way to restore a healthy gut microbiome is with fecal microbiota transplantation (FMT), a process in which fecal material from a healthy donor is transferred to the gut of a sick patient. FMT introduces a complete community of healthy microorganisms, which becomes established in the recipient’s gut, resolving the imbalance and reducing inflammation.
A growing body of scientific evidence shows that symptoms of IBD are improved by FMT treatment. FMT can be done via colonoscopy, enema, or endoscopy, but these procedures can be invasive and expensive—and in pets they frequently require sedation. Fortunately, FMT via oral delivery has been shown to be just as effective.
Gut Restore for Cats (an oral FMT capsule) is a convenient, affordable, and antibiotic-free way to reestablish a healthy and balanced gut microbiome. In a 2019 study, 83% of cats with IBD who took the Gut Restore Supplements experienced an improvement in IBD symptoms after one month.
For many cats with IBD, reducing their symptoms means a huge improvement in quality of life. Consider Marigold’s story: chronic diarrhea landed this shelter kitty on the list for euthanasia, but restoring balance to her gut microbiome resolved her symptoms and turned her life around.
Test Your Cat’s Gut Health
The best way to know how to help your cat’s individual gut microbiome is with an easy, at-home Gut Microbiome Test for Cats.
Benefits of Testing
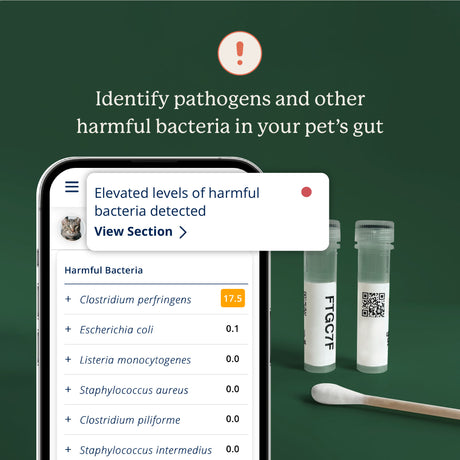
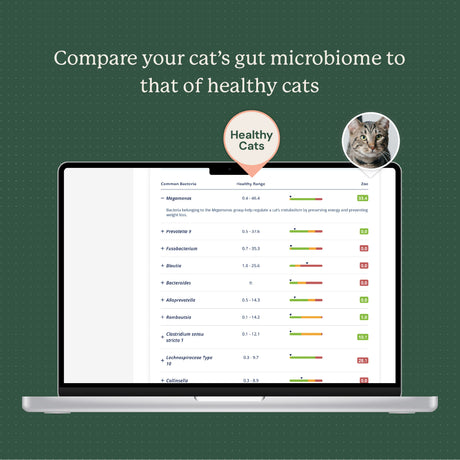
Microbiome testing uses DNA analysis to identify all the different types of bacteria in a small sample of your cat’s poop and tells you how abundant those bacteria are in their gut. A Gut Microbiome Test is a safe, affordable way to find out about possible bacterial imbalances by comparing your cat’s results to those of healthy cats. By identifying any missing beneficial bacterial groups, revealing the presence of any harmful populations, and describing imbalances of specific bacteria, microbiome testing can often help pet parents and veterinarians address the underlying condition before it leads to a chronic health issue.
Why Are Bacterial Imbalances Unhealthy?
Imbalances among the various bacterial populations in your cat’s gut microbiome can lead to inflammation of the gastrointestinal tract, and vice versa. For example, the GI tract responds to inflammation by increasing mucus production. Some inflammation-causing bacteria thrive on the nutrients found in mucus, so by feeding those harmful bacteria, the increased mucus response actually perpetuates the inflammation cycle. Many studies have found a correlation between an imbalanced gut bacterial community and IBD in a variety of animals, including cats and humans.
What Causes a Gut Microbiome Imbalance?
So how does a gut imbalance even happen? Imbalances can be caused by any disturbance to bacterial populations, such as an illness or a course of antibiotics, which can do long-lasting damage to the gut’s bacterial community. A cat’s diet can also contribute to bacterial imbalances by promoting inflammation of the GI tract.